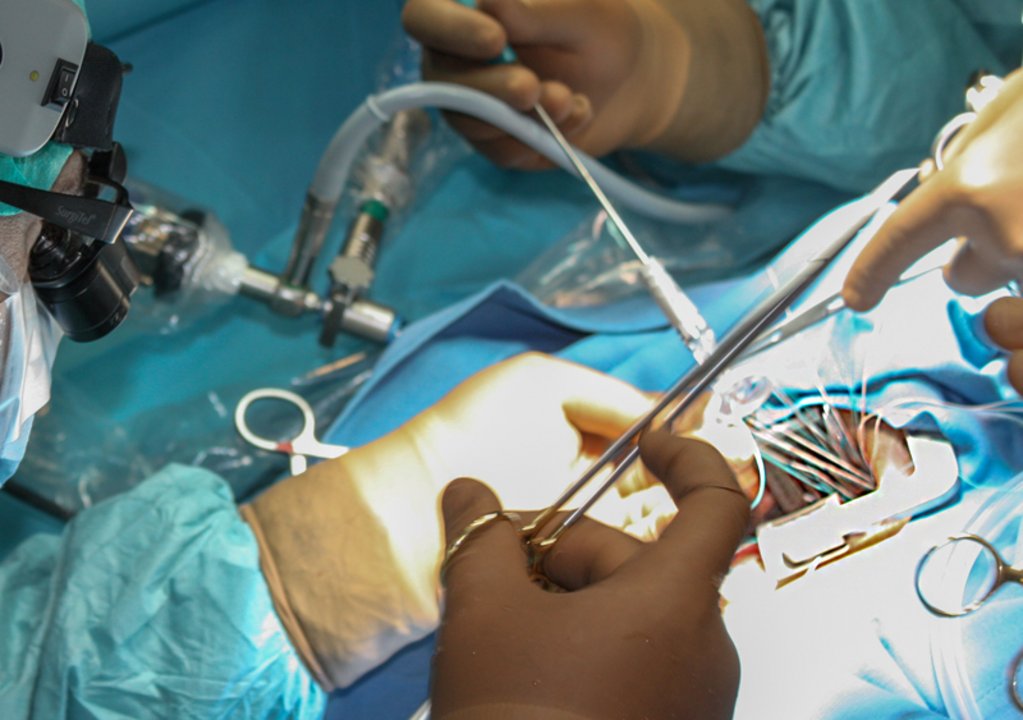
Minimally invasive procedures facilitate complex heart operations
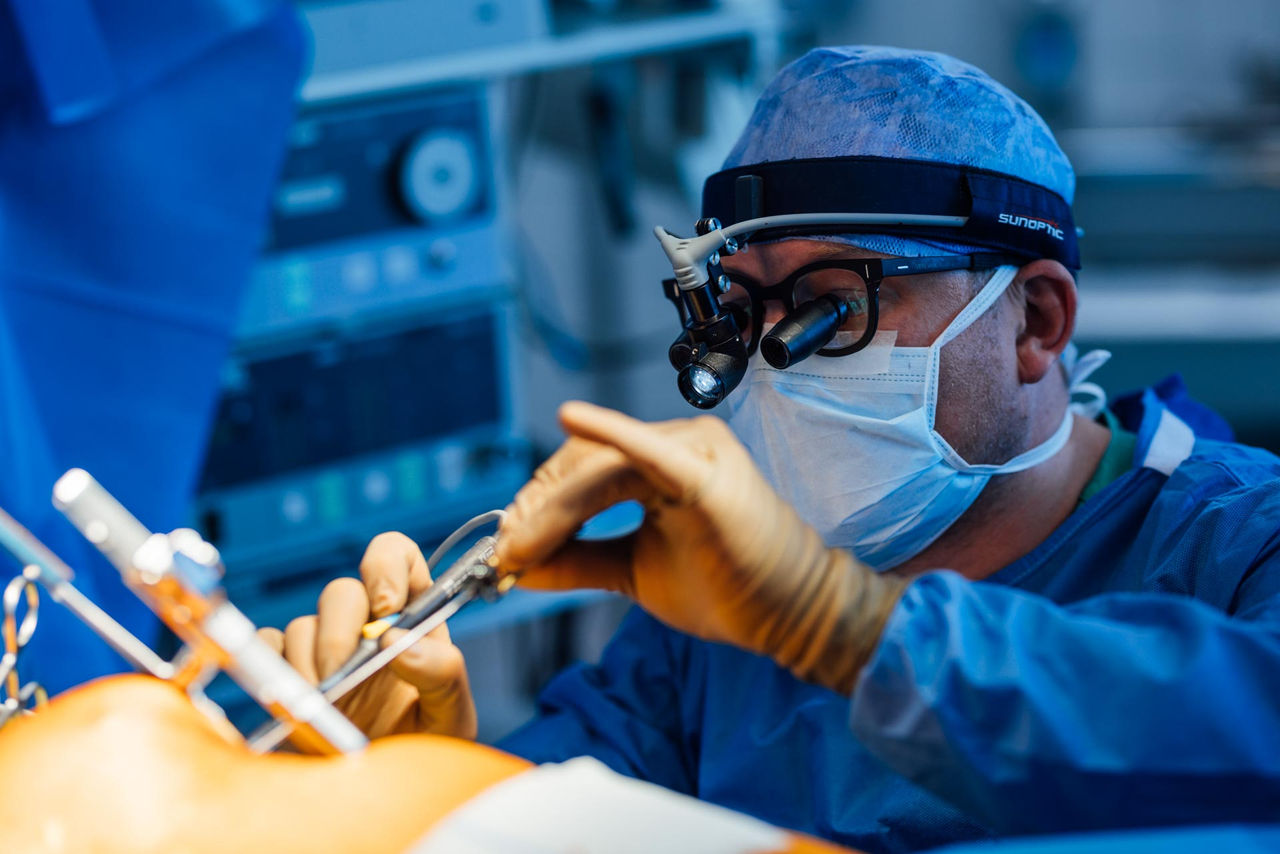
The Heart Center Siegburg rightly enjoys a position as pioneer in innovative treatment methods; not least, the cardiology department there has been distinguished as a European Center of Excellence for therapeutic procedures in catheter-interventional heart valve treatment. Quality that convinces: More than 7,000 patients receive treatment at Herzzentrum Siegburg every year. The interdisciplinary team of the Heart Center was strengthened as of June 1, 2021 with Prof. Dr. Mirko Doss as the new Chief Physician of Cardiac Surgery. With his extensive expertise, he is expanding the range of services offered by the interdisciplinary Heart Center to include various minimally invasive treatment methods such as minimally invasive aortic surgery and minimally invasive artificial heart implantation. In addition, minimally invasive procedures for reconstruction of the aortic valve are increasingly used in the clinic. Many patients can thus be spared a valve replacement. These therapy methods work entirely according to the principle: "Healing with small incisions!" - as little as possible, as much as necessary.
The minimally invasive surgical spectrum
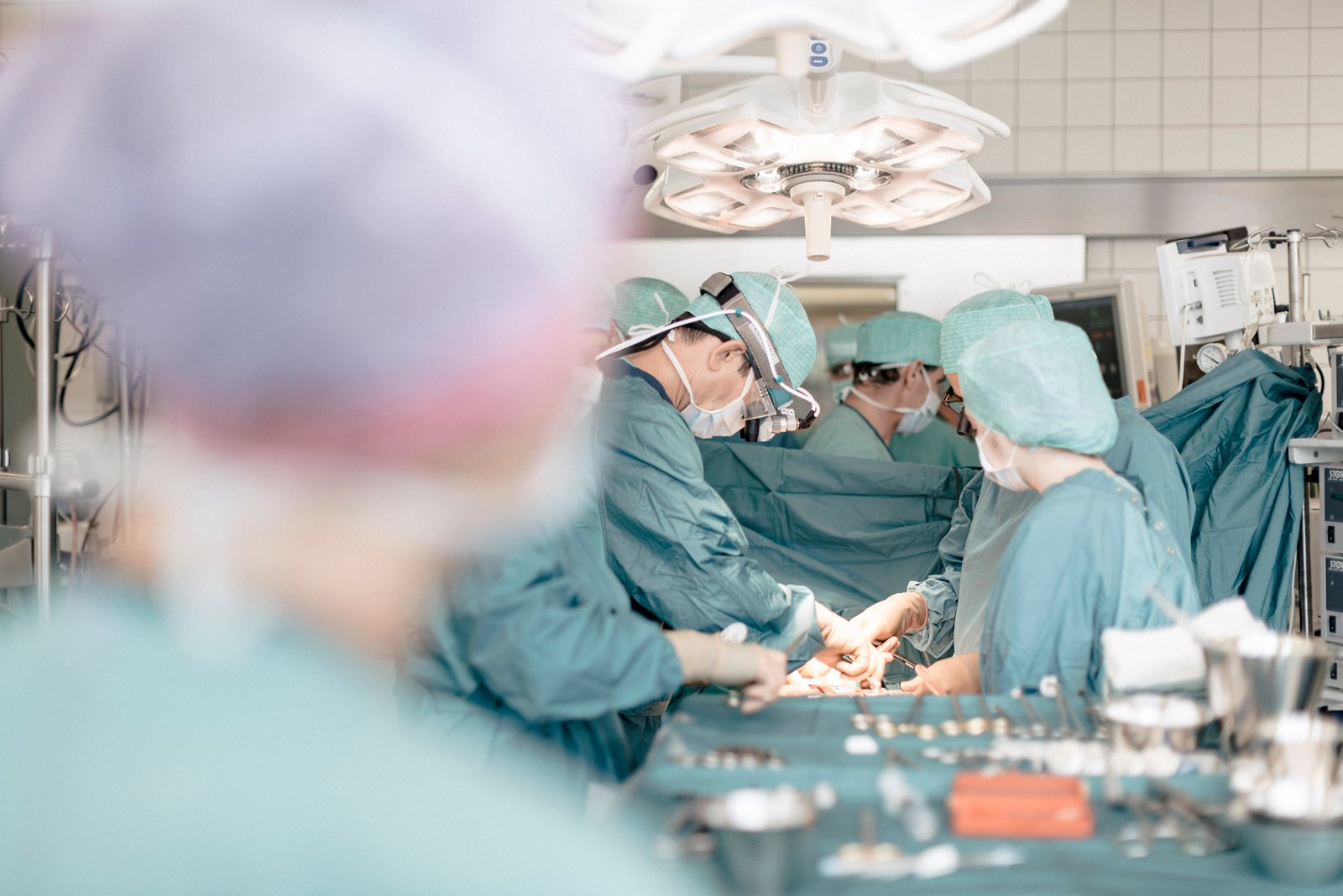
Prof. Doss and his team have extensive knowledge and international experience in the field of complex cardiac operations and combination interventions via minimally invasive approaches and procedures. Minimally invasive procedures can be used for the following indications:
- Multiple heart valve operations with reconstruction/replacement
- Replacement of the thoracic aorta and the Aortic arch
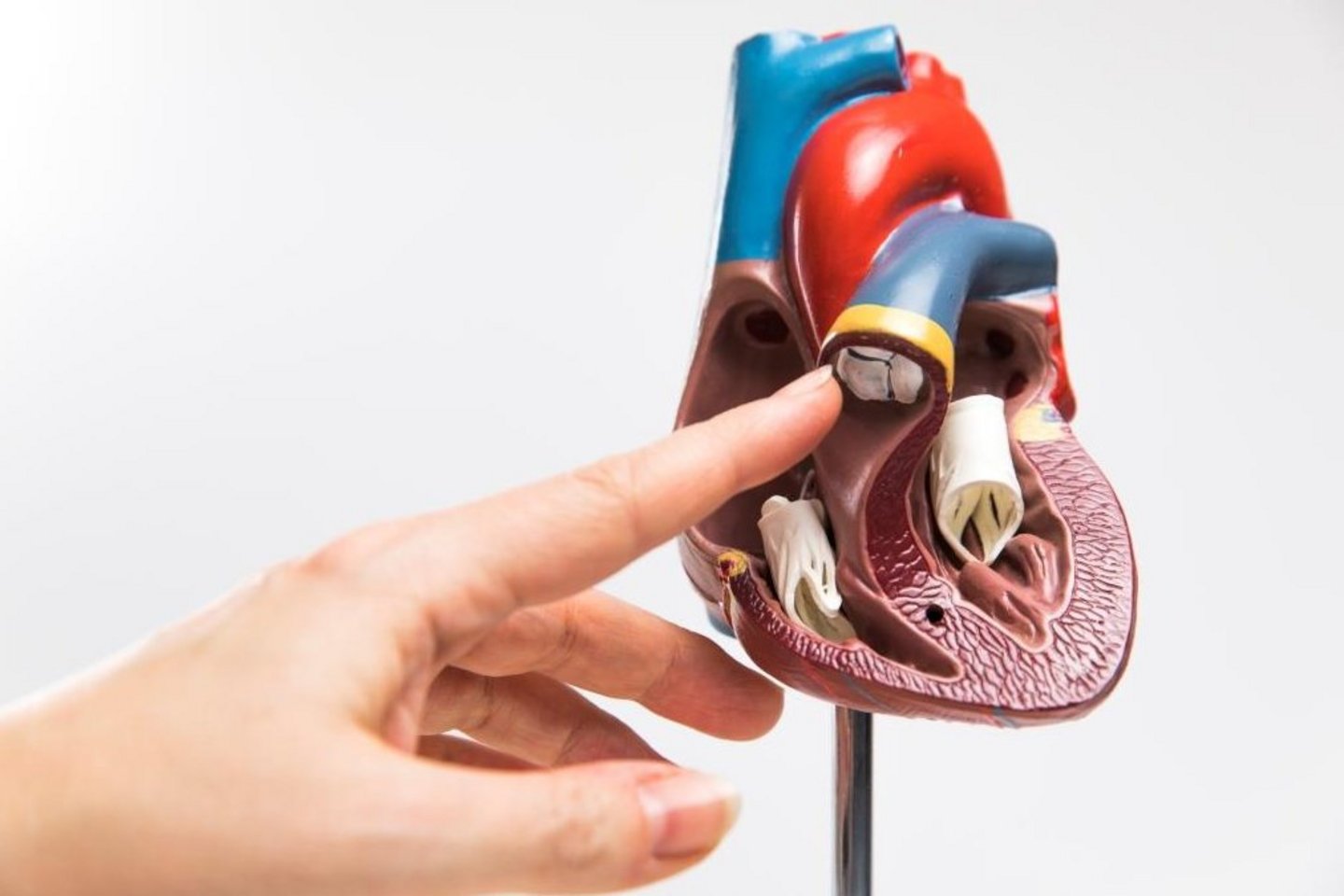
- Aortic valve and aortic root reconstructions
- MIDCAB bypass surgery
- Correction of congenital heart defects in adulthood
- Artificial heart implantations
- Excision of cardiac tumors
An overview of minimally invasive surgery
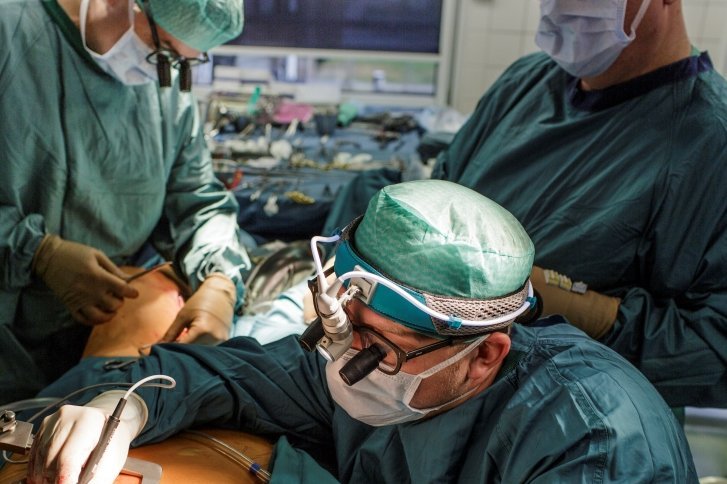
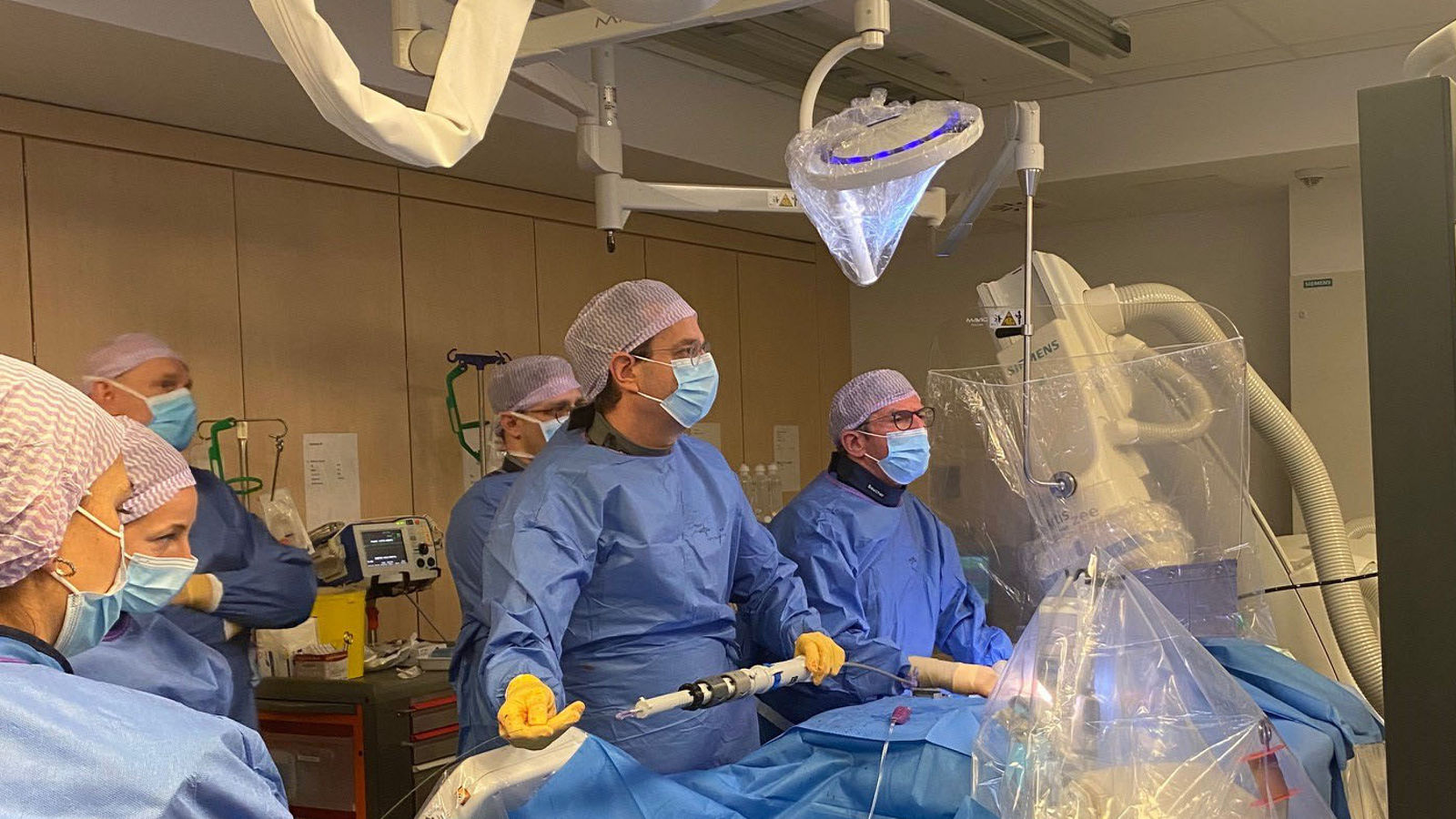
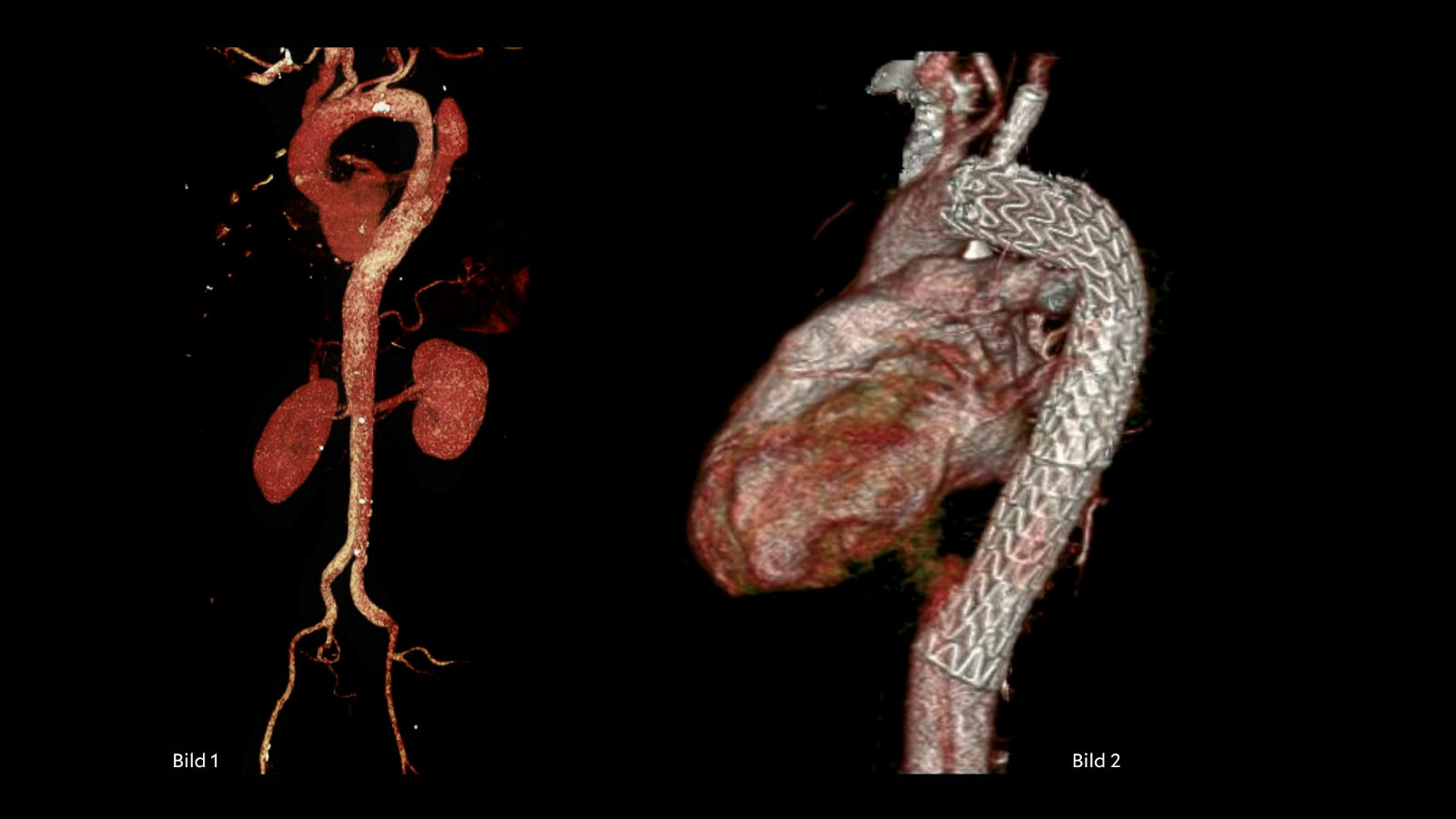
In July of this year, the team around Prof. Doss succeeded in replacing the ascending aorta and the aortic valve in a minimally invasive combined operation on the thorax - this required only a 5 cm incision. The operation was indicated by a severely calcified and congenital bicuspid aortic valve and an extensive aneurysm of the ascending aorta. This condition provides optimal conditions for the use of a minimally invasive procedure. If a combination procedure had been performed via a complete sternotomy, it would have been necessary to cut through the entire sternum, including an incision 30 cm long. However, thanks to the minimally invasive procedure, access could be made via an anterolateral thoracotomy, i.e., in this case, the sternum does not have to be cut first. In addition, a partial upper sternotomy is still possible, in which the sternum is partially opened up to the 3rd intercostal space. In both cases, the skin incision is a maximum of 5 cm long.
The advantages for patients
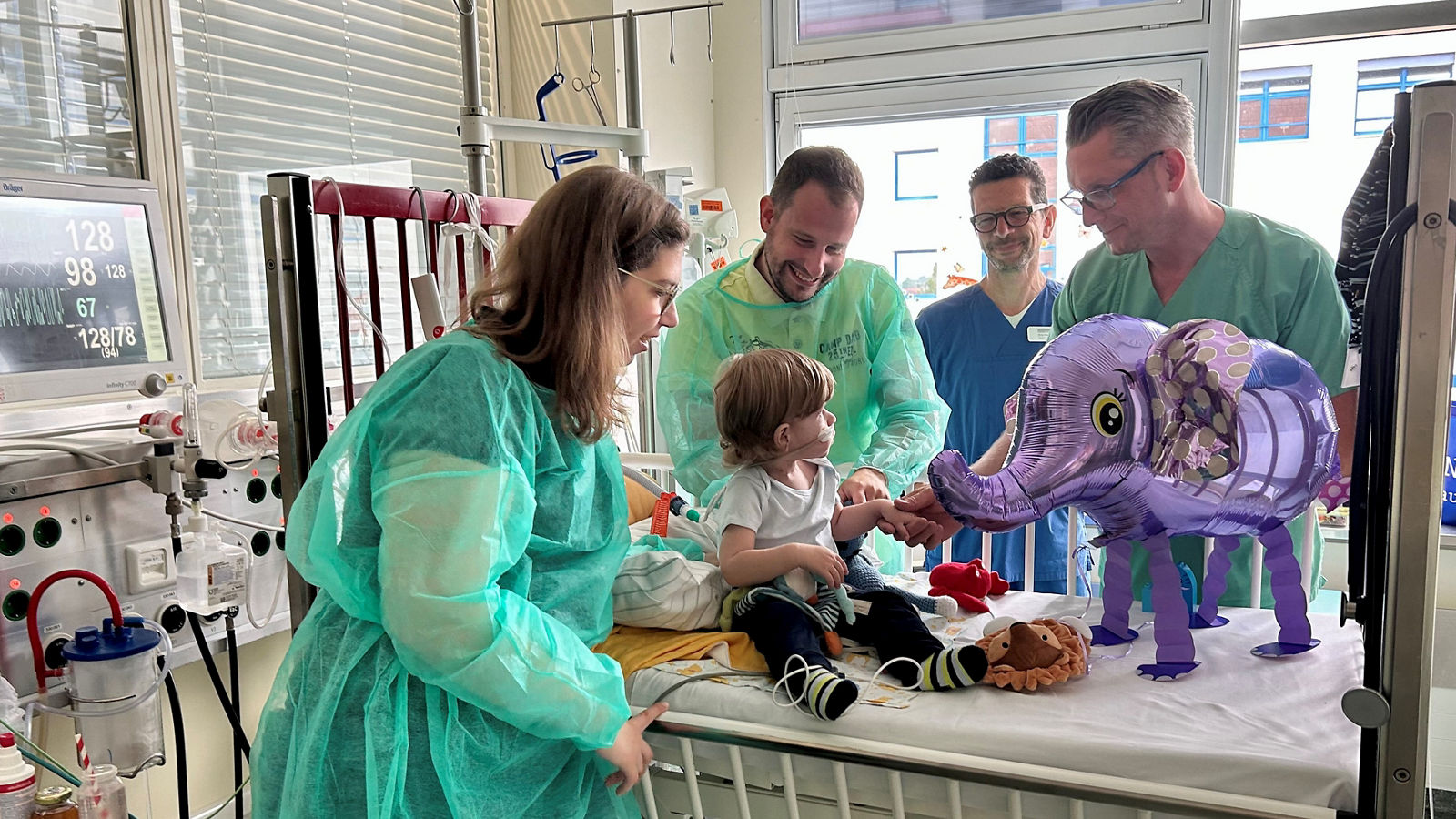
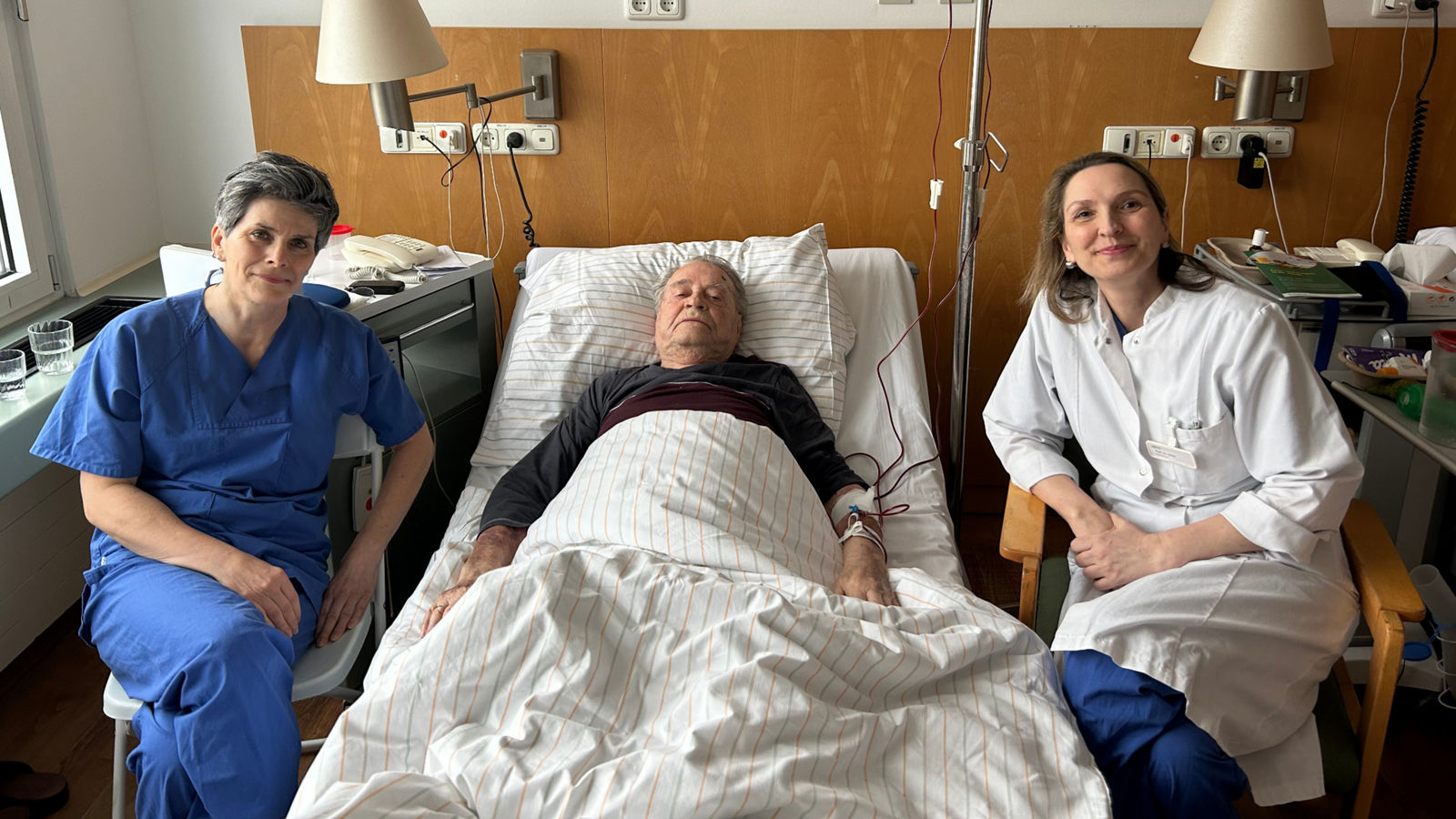
The advantages for patients are manifold. One of the main advantages is that patients experience significantly less pain and recover more quickly as a result of the minimally invasive procedure. During the procedure, patients also have to be ventilated for a shorter period of time, which puts less strain on the body. Healing after the operation is also much faster, because there is much less bleeding during the operation itself. This is also associated with a lower risk of infection. For the patient's subsequent recovery, it is also of great importance that the stability of the thorax is much higher than would be the case with the procedures commonly performed to date. In anterolateral thoracotomy, the full length of the sternum remains untouched and therefore stable. In partial upper sternotomy, the sternum is only transected in the area of the first 3 pairs of ribs and the remaining 9 pairs of ribs and costal arch remain stable. Accordingly, patients are mobilized more quickly and can leave the hospital sooner. Last but not least, the significantly reduced scar size results in a better cosmetic outcome than would be the case with conventional alternatives.
Read more:
Do you need more information about Helios Hospitals or want to schedule your treatment?