The Ozaki procedure is a good alternative to a biological valve replacement
Today we are talking to PD Dr. med. Jaroslav Benedik, senior consultant at the Clinic for Cardiac Surgery and Cardiac Vascular Surgery at Helios Hospital Krefeld, about heart valve diseases and the innovative Ozaki method
It is due to the increasing life expectancy in Germany. Here is an example: the number of people over 65 in Germany has grown from 12 million (15% of the total population) in 1991 to 18 million (22% of the total population) in 2019. This affects industrialized countries such as the USA, EU, which have strong health systems. Speaking of developing countries, the possible causes of increasing heart valve diseases are war, poverty and weak health systems.
Of course, the method of treatment is chosen based on the form and cause, as well as the pathology of the valve heart disease. For example, the reconstruction should always overtake the replacement of the valves. Other important factors are the patient wishes, the age of the patient, the lifestyle and the secondary diseases.
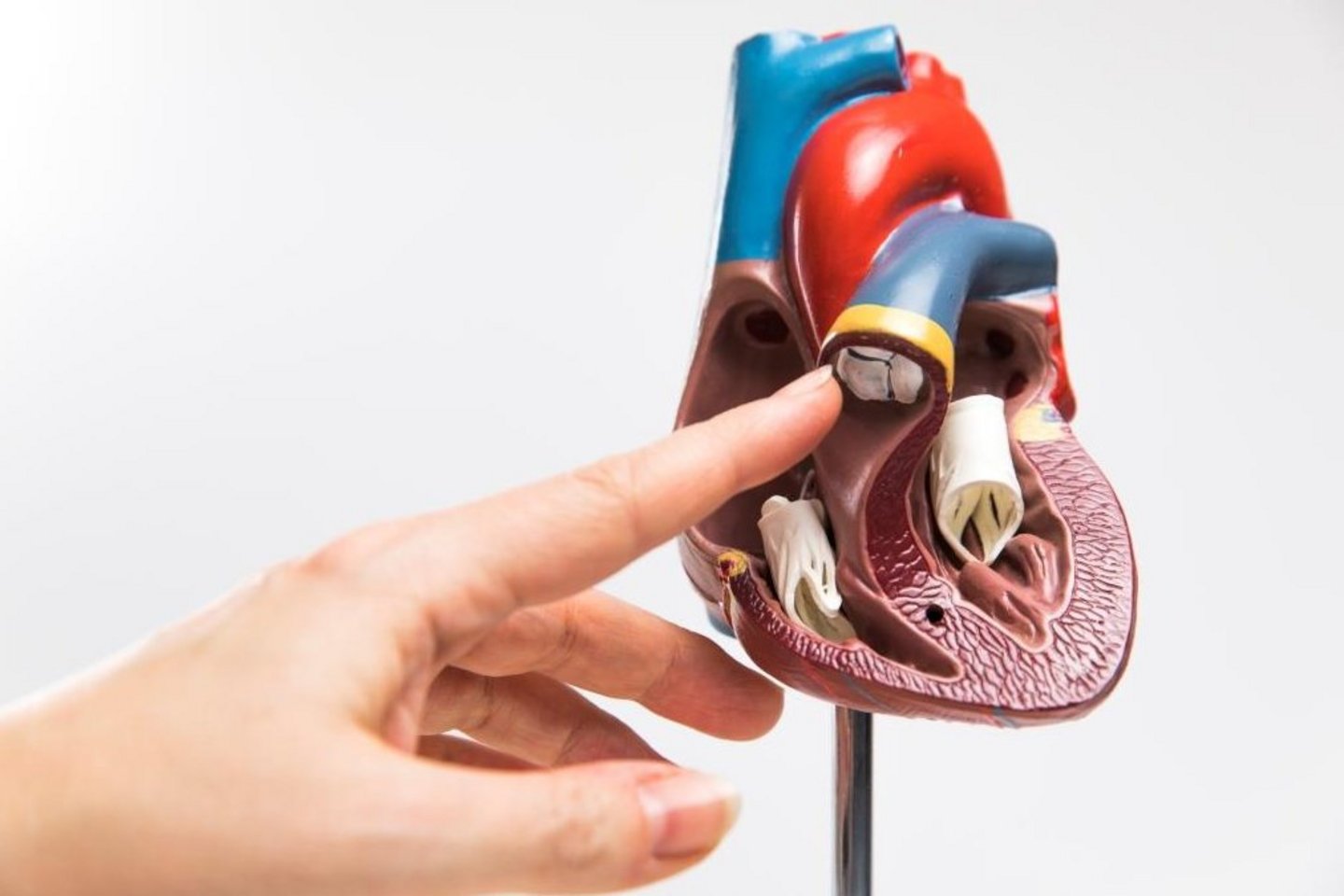
Ozaki technique is a relatively new, innovative method of treatment / replacing of the aortic valve which is irreparable. The name "Ozaki" comes from the Japanese heart surgeon Shigeyuki Ozaki, who invented and developed this type of operation. The aortic valve is replaced by its own heart sac (pericardium). The medium-term results are excellent and published in medical journals. I took over this technique from Ozaki and modified it in certain areas such as the surgical technique and the measurement method. Moreover, I expanded the range of application of the Ozaki method with Prof. Kostelka (Helios Leipzig) on the pulmonary valve.
There are many advantages. The first advantage involves using the body's own tissue to construct the new aortic valve with no immune response. Second advantage is the size of the valve and the width of the opening compared to stented biological valves (the most commonly used valve implants). The large “meeting area” of all cusps lowers the forces that could cause the degeneration (calcification, thickening) of bio-valves. The next advantage is much simpler implantation compared to stentless valves (the biological valves without a framework). The so-called TAVI (transcatheter aortic valve) is suitable for serious cases for patients, who already has been operated, or for very old patients and should not be implanted without the consent of the "heart team". Finally, the so-called Ross operation turns one-valve disease into a two-valve disease and pediatric cardiac surgeons only recommend this for newborn children, where no other option for an aortic valve is possible. The Ozaki is a good alternative to a biological valve replacement in patients with the small annulus (prevention of the patient-prosthesis-mismatch; small valve to the body) and in patients with inflammation of the aortic valve called endocarditis.
The short and medium-term results of the Ozaki valve (11-year results) and my modified Ozaki valve (2 year and 5-year results) look promising, but we have to wait for the long-term results.
This method has the great advantage that it can be used with any aortic valve disease. In particular, it is most suitable for younger patients, patients with a small annulus, patients with endocarditis. The relative contraindications for Ozaki surgery are diseases of the pericardium, e.g. calcifications, inflammation, cysts and adhesions from previous heart surgery, radiation, inflammation, which can affect the quality of pericardium used for construction of the aortic valve. Our search for replacement material e.g. bovine pericardium or tissue-engineering pericardium has so far been bound with moderate success due to the high rate of postoperative valve inflammation or so called proliferation (thickening) of neo-cusps.
"This method has the great advantage that it can be used with any aortic valve disease."
The operation can be performed on children (the youngest patient in our practice was 11 months old) up to patients aged 75 years. Pediatric cardiac surgeons are also very interested in having this method in their portfolio. After age 75, the benefits of the Ozaki operation are no longer in the foreground.
There are no specific complications after Ozaki surgery. We observe almost the same complications as after any cardiac surgery operation.
After the operation, the patient only receives 100mg aspirin for 3 months. If there are no other concomitant diseases present, the patient needs no special medications afterwards.
There are no differences from traditional aortic valve replacements. The healing of the wound and the sternum also take a similar amount of time. The absence of 8x8cm removed own pericardium does not cause any problems.
The preparation for the operation doesn’t differ from other heart surgeries. The operation usually takes 3-4 hours. Harvesting of the pericardium take about 15 minutes. After the aortic valve has been removed, the measurement comes with special instruments. These templates are then used as patterns for new cusps. Each cusp could have a different size and the congenital bicuspid valves are usually (99%) converted to normal tricuspid valves. Every cusp is then sewn separately to the annulus with the suture. The commissures (meeting points between cusps) are constructed with additional suture and proper length is adjusted with the help of world-unique three-armed forceps. All of the work takes about 70-80 minutes from cardiac arrest. For your comparison, the uncomplicated aortic valve replacement by complete sternotomy takes an average of 50-60 minutes of cardiac arrest. The finished valve is checked with a transesophageal echo after the weening from the heart-lung machine.
The postoperative course does not differ from other heart surgeries. Follow-up care includes annual transthoracic ultrasound for all patients.
For an uncomplicated operation with completed preliminary examinations, the foreign patient must plan around 10 to 12 days. As with every heart valve surgery, a visit to the dentist should be carried out before the surgery.
Unfortunately, there are no statistics yet. Since this method is relatively new and can only be carried out in very few centers worldwide. The possible causes for re-operation are the degeneration of the new Ozaki valve or an infection of the new valve (neo-valve endocarditis). According to our observation and the data published so far, the valve endocarditis after Ozaki procedure with own pericardium tends to be less in comparison to other standard valve prostheses. Till now we have expected no calcifications or thickening of the valves has been found after the Ozaki operation. However, increased valve deterioration has been reported by using substitute material e.g. bovine or horse pericardium.
In recent years we have performed around 50 Ozaki procedures per year. We are often consulting patients who live outside of North Rhine-Westphalia regarding this procedure. For every interested patient, there is no limitation in waiting time. The patients outside of our region have priority in fixing an appointment. Theoretically, we can perform two procedures a day in regular working hours. Foreign patients are always welcome.
"In recent years at Helios Krefeld we have performed around 50 Ozaki procedures per year."
I have been practicing this method since September 2015. I was involved in the development of measuring tools and also the special forceps. The second part of the question is very difficult to answer because each method always has its advantages and disadvantages. The patient together with the doctor should bring the importance of those on the scales and decide.
Yes, sure. Nowadays we operate on significantly older and sicker patients. Every day we have to reckon with increased risks of comorbidities.
Can you please give us an example of one of the most interesting patient stories in your practice?
There are many interesting situations during operations as well as the operations themselves. The most unique of these are usually relatively simple surgeries that no one wants to perform for fear of failure and patient death. In such cases, I allow myself to be guided by my "sixth sense". One patient was admitted for coronary revascularization and the pump function of the heart was no more than 10%. All cardiologists and cardiac surgeons were against the operation, only I agreed to the operation. I discussed the plan of the operation with the patient and his relatives. The operation took place without complications. The patient was discharged home in good condition with a pump function of 35% on the 7th postoperative day.
I've been engaged in cardiac surgery since I saw my first heart operation in the first year of my medical school. Since then I have spent all of my free time preparing for a career in cardiac surgery. I was interested and open to all new methods that can help my patients. That's why I chose the most difficult valve to repair (the aortic valve) and specialized in this area. The aortic valve repair/construction (Ozaki) also includes the immediate surroundings - aortic root and aorta so these are also part of my expertise.
I like golf, unfortunately now I have no much time for it. Otherwise, I relax while walking my dog.
The hardest question at the end. I see the future in close cooperation with cardiology and vascular surgery. Only with very close cooperation and strictly “evidence based” decision making, and also centralization of “special” procedures in high volume centers could improve our results.
Read more:
Do you need more information about Helios Hospitals or want to schedule your treatment?