The Fontan principle is a long-term treatment solution for children
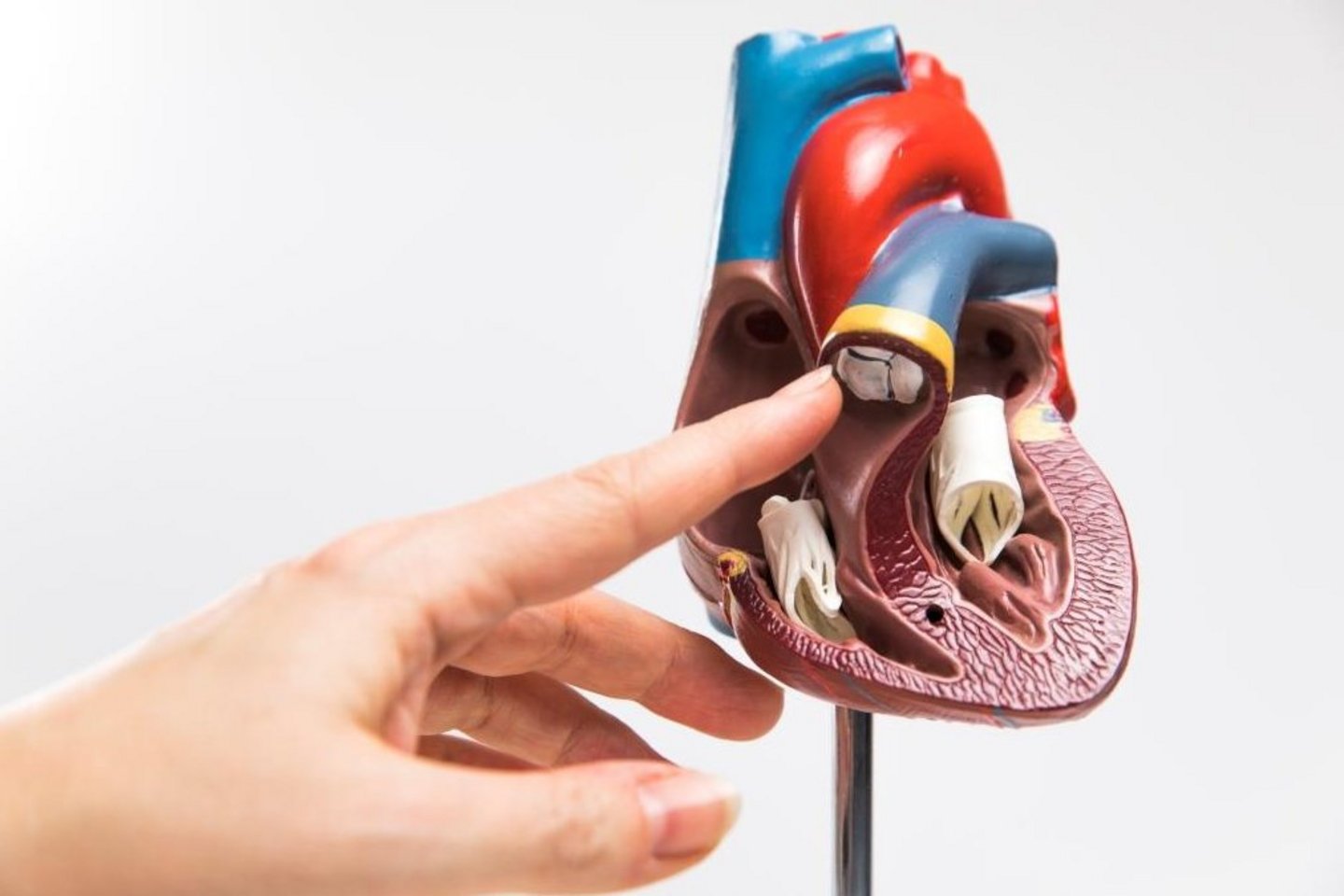
Today we are here together with Prof. Dr. Ingo Dähnert, Director of the University Clinic for Pediatric Cardiology at the Helios Heart Center in Leipzig, talking about congenital heart defects and the most common types of surgical treatment in pediatric heart surgery including the Norwood, Glenn and Fontan procedures.
Congenital heart defects are rare. According to statistics, only around 1 percent of children is born with them. We do not yet know exactly why they occur.
Congenital heart defects are usually disorders of the embryonic heart development in the first eight weeks of pregnancy. Only in a few cases, heart defects can be caused by certain known genetic defects. In most cases, however, congenital heart disease is most often an unfavorable combination of several genetic factors, each of which does not individually cause the disease.
Compared to the past, today certain diseases (e.g. rubella) an early pregnancy stage rarely lead to congenital heart defects. Finally, there are congenital heart defects that arise due to the fact that the necessary compounds that are formed in the womb and should be closed after birth, do not “close”, but remain “open”.
"According to statistics, only around 1 percent of children is born with congenital heart defects"
The development and function of the heart is assessed in all antenatal examinations. If there is a suspicion of a congenital heart defect, it can be ruled out or identified and accurately described using a detailed diagnosis (usually from about the 20th week of pregnancy). Today we also know that some congenital heart defects change during pregnancy, which can lead to progression (an increase in certain narrowing of the valve) or even regression (a decrease in the size of the openings in the interventricular septum). Not all heart defects can be diagnosed prenatally; the compounds mentioned above (the opening in the middle of the interatrial septum, the connection between the body and the pulmonary artery), become heart defects only if they do not close after birth. The statistics on prenatal diagnostics of congenital heart defects in Europe show a wide range from 20 to 90 percent, both depending on the type of heart defect, regional rules for diagnosis and individual conditions of care. In Germany, in addition to prenatal diagnostics, newborn screening with pulse oximetry and pediatric examinations are used to detect congenital heart defects.
No, not all congenital heart defects require surgery. Surgical interventions are necessary for the so-called complex heart defects; the need for intervention for other heart defects depends on individual characteristics. Often, regular examination and observation is sufficient. In some cases, with certain heart defects, even self-healing after childbirth may occur (for example, spontaneous closure of certain defects of the heart septum), or the changes remain so minor that they do not pose a threat.
It depends. In some cases, the operation is absolutely necessary for the newborn (so-called critical heart defects), in others it is even possible to wait until adulthood (for example, with Ebstein's anomaly). For some complex heart defects, it is clear from the beginning that one operation will not be enough, and the treatment will include several surgical procedures.
What are the most common surgical treatments of congenital heart defects worldwide today?
In principle, a distinction is made between interventions where it is necessary to open the patient's chest (operations with or without a heart-lung machine), and operations in which the intervention can be performed through blood vessels (so-called "catheter interventions"). Operations that combine both methods are called "hybrid" interventions. The decision about what kind of operation is indicated for a particular patient is made in each case individually.
In 2019, the Heart Center Leipzig performed 9 Norwood operations, 15 Glenn operations and 10 Fontan operations. All operations were successful. This is not always the case: in total, in 2019, 6 patients from more than 1,000 inpatients with congenital heart defects died at the Heart Center Leipzig. Among them was one child with Left Heart Hypoplasia Syndrome (HLHS), an interrupted esophagus and other problems. It was decided together with the parents not to have the operation.
"In 2019, the Heart Center Leipzig performed 9 Norwood operations, 15 Glenn operations and 10 Fontan operations. All operations were successful".
From a medical point of view, the treatment of congenital heart defects in Germany does not differ from the treatment in the USA, Israel or other European countries. The only difference is the organization of medical care and prices.
About 1000 children from Germany with congenital heart defects are being treated annually at the Heart Center Leipzig, but families often come from abroad in order to treat their children here. Most of them come from Eastern Europe and Africa, where suitable CHD treatment is not available.
At the Heart Center Leipzig, Fontan surgery is usually performed with an extracardiac conduit without fenestration, and our experience has shown good results. Fenestration is only used when certain risk factors are present.
What does a good life mean? The Fontan principle is a long-term palliative treatment for children with congenital heart disease. It is impossible to correct these defects, because there is still no method for creating a second heart chamber anywhere in the world. Even with the Fontan operation, the consequences of these serious malformations cannot be completely eliminated, but they can be significantly alleviated. In many cases, this means that a good quality of life is possible over a long period of time. Going to school, studying, doing normal work and sports is usually possible. On the other hand, regular check-ups and often lifelong usage of one or more drugs is required. If young women with congenital heart disease, for example, want to have children, they need to discuss this individually with their doctor and assess the risks based on the current results of the next examination. Absolute restrictions usually apply to participation in sports competitions and professional sports, as well as work involving heavy physical activity (for example, a construction worker, foundry worker, mountain guide) or to special health requirements (for example, a pilot or diver).
"The Fontan principle is a long-term palliative treatment for children with congenital heart disease".
Norwood's operations have only been regularly performed at the Heart Center Leipzig since 2000, so our “”oldest patients with left heart hypoplasia are now 21 years old. As for the patients after the Fontan operation, here our patients with other heart defects (for example, with tricuspid valve atresia) are now between 40 and 50 years old. In total, we are now observing and providing care to almost one hundred adult patients who have undergone Fontan surgery.
"We are now observing and providing care to almost one hundred adult patients who have undergone Fontan surgery".
If the condition is stable, we recommend annual cardiological examinations by a pediatric cardiologist or GUCH cardiologist, i.e. a specialist for adults with congenital heart defects. In addition to the physical examination, this examination also includes blood pressure measurement, pulse oximetry, an ECG and an echocardiography. Exercise tests (spiroergometry), long-term ECG, liver elasticity measurements and blood tests are recommended at longer intervals. X-rays and coronary arteriography, which are mandatory before the Glenn and Fontan operations, are not indicated anually and are performed in special cases only. We recommend to perform an MRI only after the Fontan surgery and only as frequent as every 5 years later on.
Yes, it does. There are protocols for treatment before Norwood surgery, for performing Norwood surgery, and intensive therapy afterwards. There are further protocols for the "interstage" phase between the Norwood and Glenn operations, the Glenn operation (Norwood II) and its pre- and post-treatment, and the Fontan operation. Of course, these protocols have to be adapted individually for each patient.
Indeed, both complications are very serious, but fortunately rare. The frequency of their occurrence is overestimated, since they appear almost only after the Fontan operation. In Leipzig, for example, we are currently treating one patient with plastic bronchitis and two patients with protein enteropathy.
Annual examinations are not required for this. Unless otherwise specified, the examination intervals between the liver elasticity measurements and blood tests can be between two or three years.
The annual examinations after Fontan's operation are carried out by an experienced pediatric and senior GUCH cardiologist, who also heads the outpatient department. In case of any anomalies, the other specialists at the clinic (rhythmologist, catheterologist) or the chief physicians are involved. The findings are discussed together with parents and the further procedures are planned.
The examination program for foreign patients is usually planned in advance. Therefore, it is especially important that we receive a report on the patient's condition, progress, any problems observed in the home country. We determine in advance whether the examination program should be carried out on an outpatient basis or in a hospital. Usually the outpatient program is designed for one day, if longer-term examinations are needed - for two days. If there is a need for a hospital examination, we also try to inform in advance about the planned hospital stay.
First, we are interested in everything, and we want to know what happened with our patient at home and what examinations were carried out. All the results are really important and interesting for us! Specific examinations are recommended individually, for example, in some cases it may make sense to do a long ECG or to determine certain blood parameters before arrival, but this is not necessary for every patient. This is decided rather individually in each case.
"All the results are really important and interesting for us!"
There are a lot of such positive stories that make our work one of the most beautiful in the world. One of the last stories: one of our first patients with left heart hypoplasia gave birth to a healthy baby: mom and baby are doing well! We are happy for a young family.
Every patient is a person and not a case. A successful treatment is work and rest at the same time: we can see a child who smiles again or a family who sends a happy picture. The negative results of our work and the complications are humiliating and unpleasant, but we are not gods. We can only ask ourselves in such cases: "What can we do better?"
Each of us has our own concept of relaxation and recovery: jogging, hiking, cycling, boating, gardening, meeting friends, a glass of wine and much more.
Please live a normal life with your child and trust your pediatrician, your pediatric cardiologist, and above all – believe in yourself!
"Believe in yourself!"
Read more:
Do you need more information about Helios Hospitals or want to schedule your treatment?