Patient Story: from the prostate cancer and operating table back to life
"The disease is for others, it will never happen to me." Many people think so, Peter Springer was one of them. Until he was also exposed to it. Peter is a little over sixty, he is a sporty, active man. He works in a hospital and cares for patients with severe pain symptoms, some of whom have recently undergone surgery. In his work, he took the fate of some patients to heart but did not expect that someday he himself would be affected. Because a serious illness did not fit into his lifestyle at all.
A close friend's illness makes you think
“I have always had a very active lifestyle. I often ride my bike to work, go jogging, go on vacation,” says a sucker for Greece. When his friend was diagnosed with prostate cancer, he was persuaded to undergo cancer screening too. “I just wanted to get it out of my head. But I didn't expect to get sick myself." In February 2019, at an appointment with a urologist, he had a blood test for PSA marker. PSA stands for “prostate-specific antigen”, the value of which must be less than 3. Peter's test was more than 5. “I have never thought about it before, sometimes the value rises, for example, due to long bike rides,” he explains. The urologist recommended coming back for a follow-up appointment in three months.
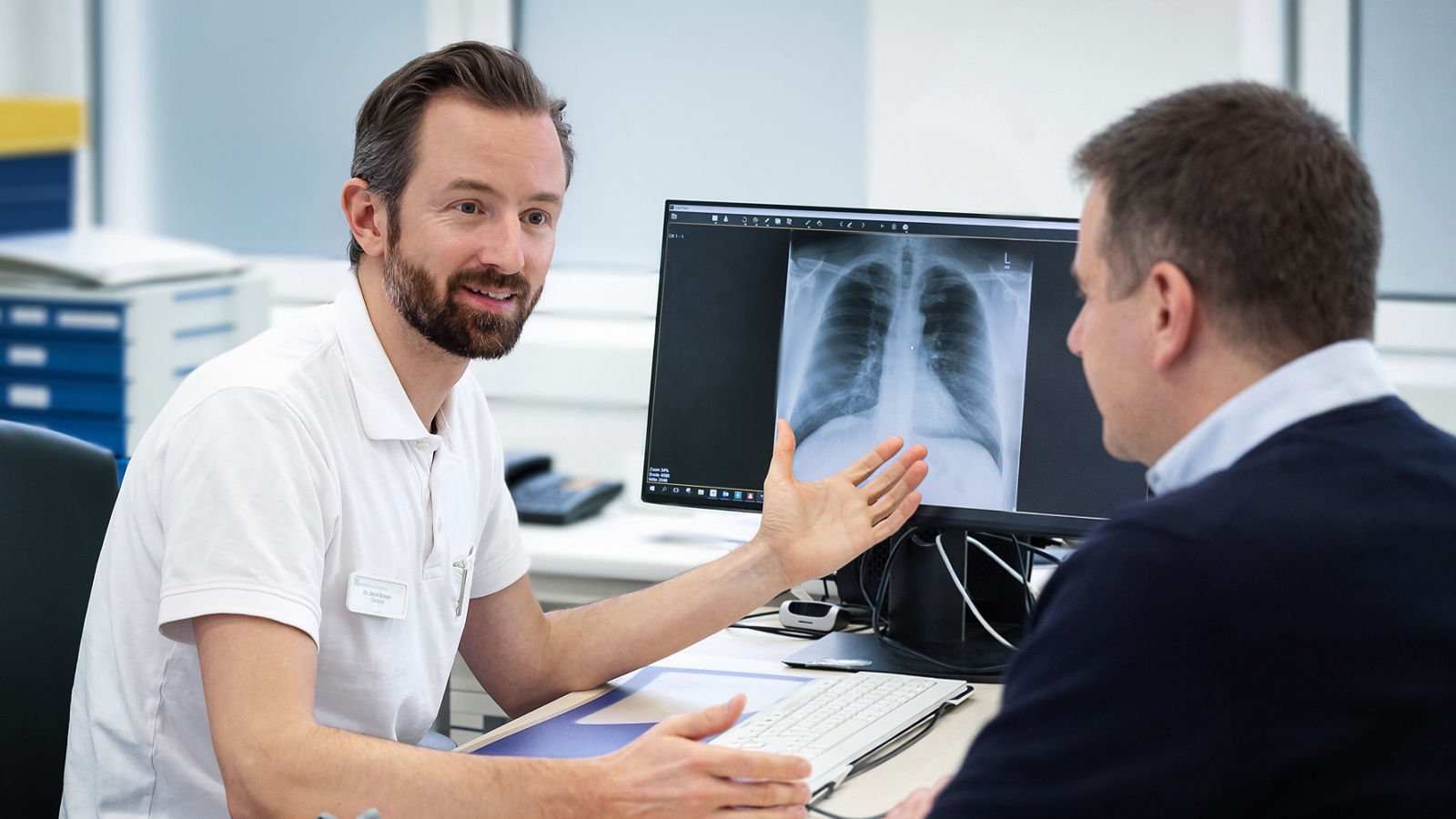
No sooner said than done: in May 2019, he was re-tested. Result: again value that is significantly higher than normal. “And then you start to think, your own dynamics develops. I asked myself: if you are really sick, what will you do?" To clarify the cause, the doctor refers him to an MRI of the prostate gland.
Diagnosis - Prostate Cancer
It was at this point that a healthcare professional first told the family about the suspicion. The news shocked his daughter: “She thought that my end was near. I have a secondary medical education, I managed to set her mind at ease."
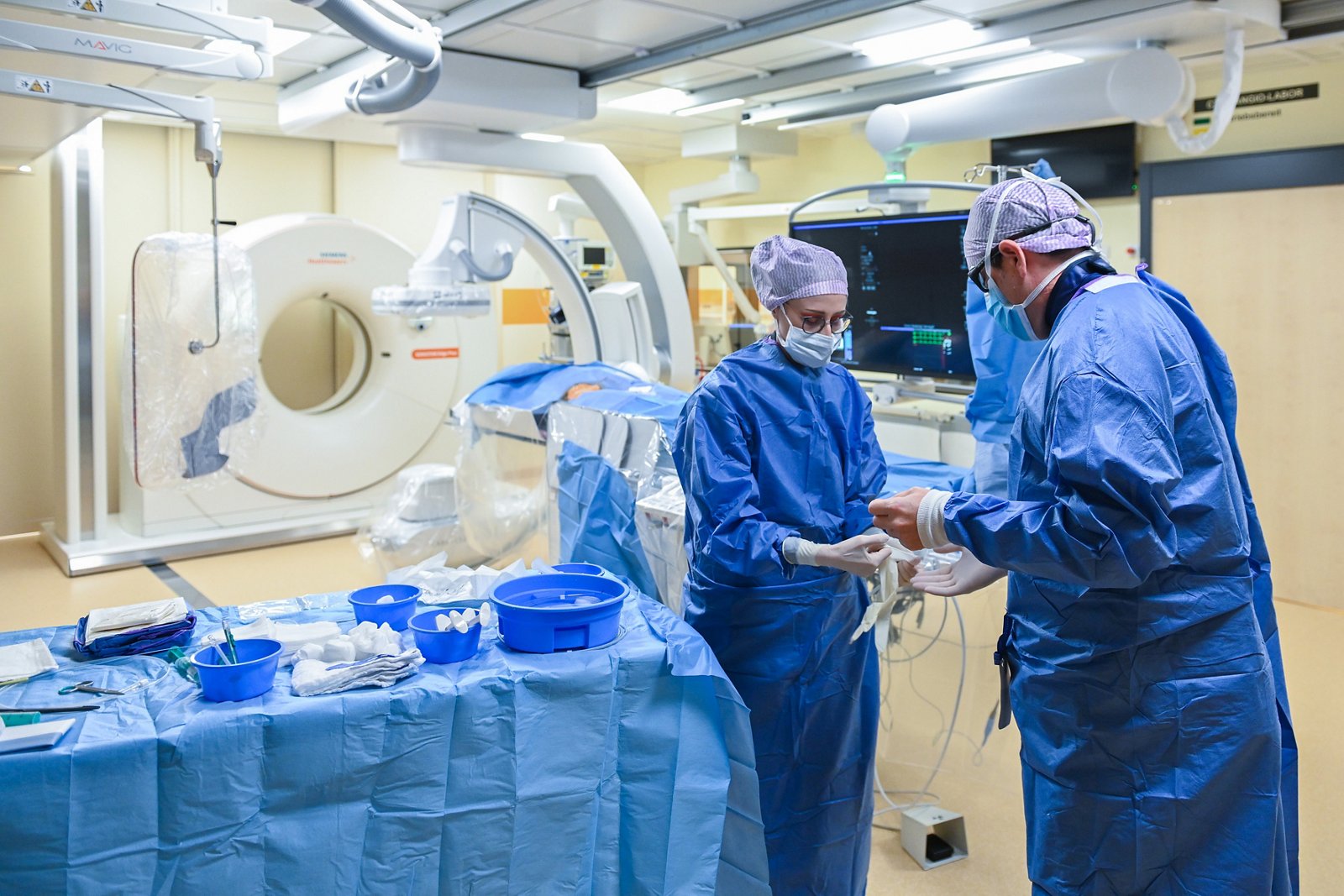
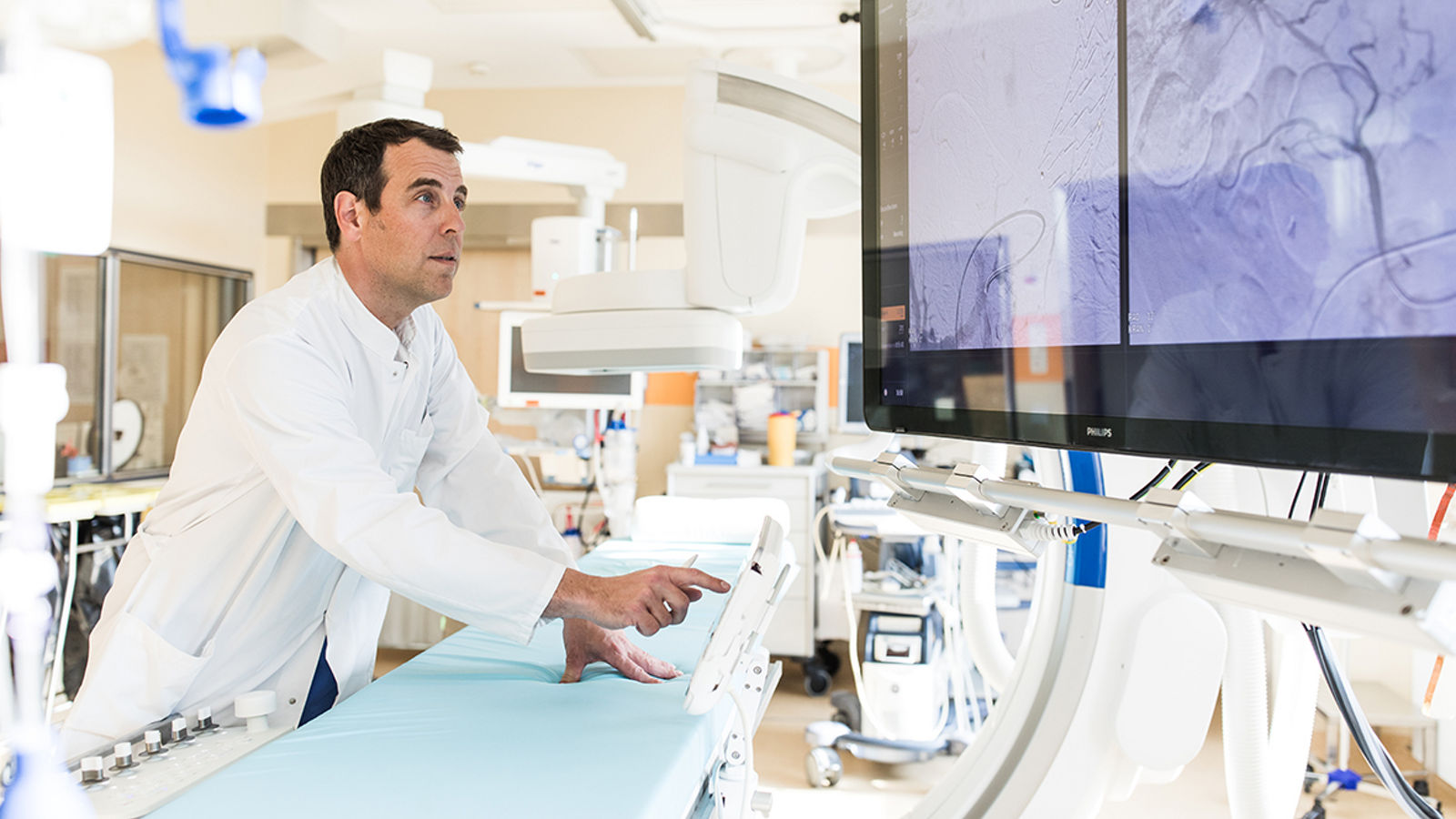
The MRI revealed and showed two abnormalities in the images – a bad sign. Since these two deviations were not yet an unambiguous result, he made an appointment with the head of the urology department of the University Hospital Helios Wuppertal, Dr. André J. Pantaleon for fusion biopsy. For the biopsy, the doctor compares the MRI scans with suspected tumor areas with the real-time ultrasound images. He takes material from the patient directly from suspicious areas and sends it for a test. The suspicion was confirmed – Peter had tumor, prostate carcinoma. He was shocked.
In order to rule out metastasis to the bone, skeletal bone scintigraphy was performed. Finally, the good news was that Peter had no metastases. CT scan of the abdominal cavity with contrast enhancement confirmed the result of scintigraphy: no data for metastases were obtained, the tumor was delimited locally.
Further therapeutic measures in close cooperation between doctor and patient
The operation was inevitable. Chief Physician Prof. Friedrich-Carl von Rundstedt explained the therapeutic options to the patient and proposed a special method: a robot-assisted operation using the da Vinci surgical system.
“The advantage of robotic-assisted prostate surgery is that it is minimally invasive,” explains von Rundstedt. “Instead of opening the abdomen with one large incision, we can use da Vinci to limit ourselves to six small incisions. Through these incisions, thin guide tubes are inserted through which we can insert microsurgical instruments connected to the robot and simply replace them if necessary." Instruments and arms are controlled from a kind of console located next to the patient. This is especially important in prostate procedures, as the risk of damage to adjacent organs and nerves is minimized.
“The advantage of robotic-assisted prostate surgery is that it is a minimally invasive method of intervention.”
– Prof. Friedrich-Carl von Rundstedt, Chief Physician | Helios Hospital Wuppertal
The complexity of the case of Peter Springer: in 2003 he underwent bladder surgery, which also affected the prostate gland. The scars from the old surgery could have jeopardized the use of the da Vinci surgical system. But the Head Physician von Rundstedt said there was nothing to worry about. He recommended immediate intervention within the next three months.
“After the explanatory conversation, it was clear to me that I want to end this whole story as quickly as possible,” the patient recalls. The time before the operation was especially difficult for the healthcare professional. “I myself have looked after patients who had extensive bone metastases because the cancer was diagnosed too late. When my back hurt before the operation, I was already thinking about it." But the fears proved unfounded.
Surgery to remove the prostate gland
In September 2019, it was time for the operation. Chief Physician von Rundstedt and his team removed the prostate completely and pelvic lymph nodes, using a robotic surgical system to preserve the neurovascular bundles that are responsible for urine flow and erectile function.
However, as with any surgery to remove the prostate gland, a urinary catheter was inserted. “You have to imagine that the prostate gland is closely connected with the bladder and urethra, that it supports them and therefore is largely responsible for good bladder function,” says the chief physician. Removal of the prostate gland can lead to impaired bladder emptying, which can usually be controlled with pelvic floor training. To improve the healing process, a urinary catheter is used, which is usually removed after about two weeks.
Peter Springer's recovery dynamics were so well that within a few days after leakage testing he could do without a catheter: “I was very grateful to the chief doctor for that!” The operation went well for him. “At first after the surgery, I must have looked terrible,” Springer says with a wink. "During the intervention, you are in a position upside down at about 30 degrees, which makes your face swell a lot." However, after a few days, the edema completely resolved.
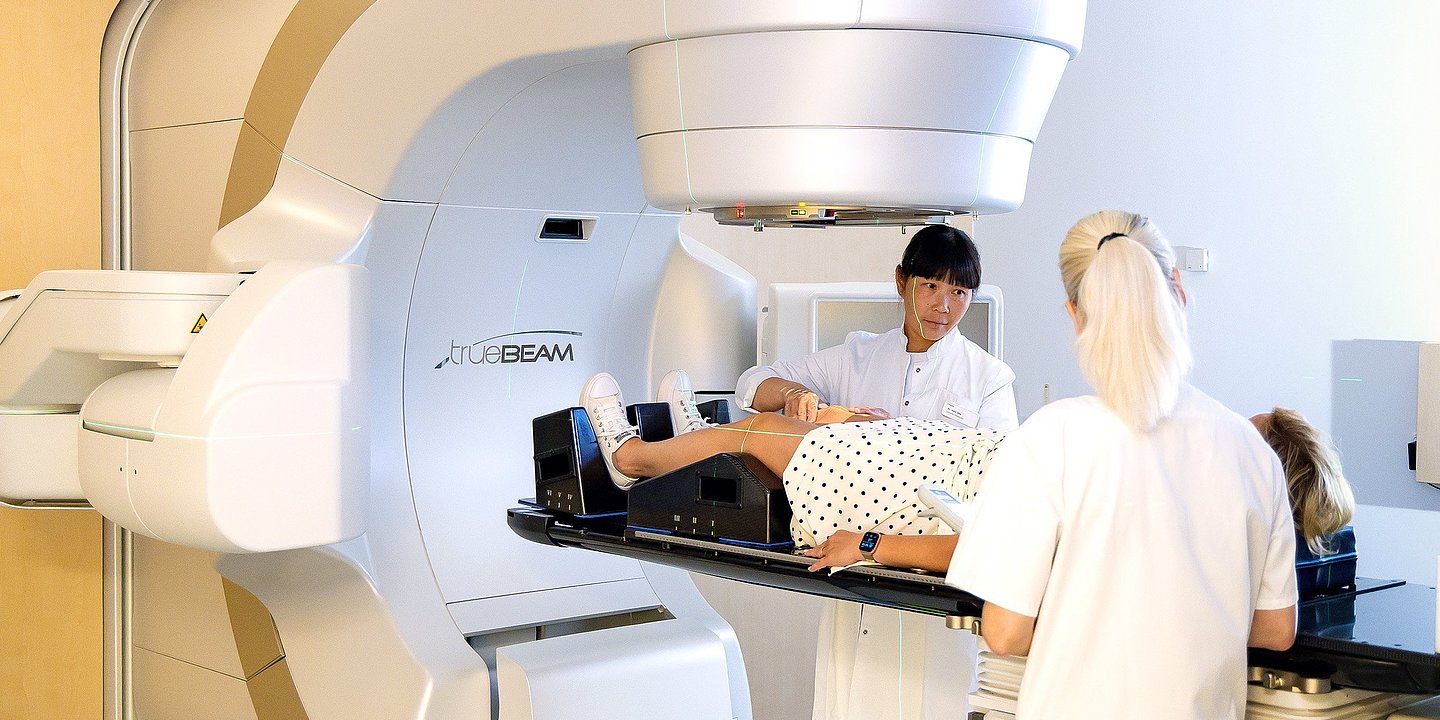
To make sure that there was no metastasis, a pathological examination of the removed tissues was performed. In general, everything was OK, but one lymph node was positive: a small metastasis formed inside it. “However, it was so small that we didn't have to take any further action,” says Friedrich-Carl von Rundstedt. If there are large lesions, the patient is given a course of radiation or chemotherapy. Peter was lucky to avoid it.
"I was happy to get back to people and a normal life."
– Peter Springer, patient at the University Hospital Helios Wuppertal
Final rehabilitation and postoperative follow-up
The operation was followed by a three-week rehabilitation in Bad Gandersheim, Lower Saxony. The main focus here is on training the pelvic floor to stabilize the ability to control urination. “The first time after the intervention, I had a constant urge to urinate, I had to use urological pads so that there would be no “accident” with a wrong movement,” the patient recalls.
But his time in rehab did him good. He was unable to work for a total of four months before fully returning to work again. "I was happy to get back to people and a normal life."
Regular monitoring of blood counts
Peter Springer is now doing well again. A blood test will be done every three months to monitor PSA, which has been normal since the surgery, so no further treatment was required. He can return to his hobbies and go on vacation. Only with certain movements does he periodically feel that something has changed, but this does not bother him. His attitude towards life changed after the diagnosis: “First of all, I made all male relatives undergo cancer screening,” the healthcare professional says, laughing. He lives a more conscious life, he no longer worries or grieves over many things. He is very grateful to his doctors: "My present serene life and the successful outcome is only thanks to the joint work of Dr. Pantaleon and Professor von Rundstedt."
He advises everyone to undergo cancer screening in a timely manner. Because with some diseases, at an early stage, there are no pain symptoms, which makes timely diagnostics difficult. "The sooner cancer is diagnosed, the better the chances of recovery." This means that others also have a chance of a positive result – like Peter.
Da Vinci® surgical system
Robot-assisted surgical techniques are considered particularly gentle for patients, also because, thanks to several small incisions, the recovery time is shorter compared to conservative surgical methods. At the University Hospital Helios Wuppertal, the da Vinci surgical system has been used in urology since May 2019 and is now being used in other departments such as gynecology and visceral surgery.
For interventions using the Da Vinci system, a computer with precision devices maintains the surgeon's arm movements in a balanced manner, and also significantly increases the range of movements. Thanks to a large number of degrees of freedom, i.e. extremely maneuverable tools, new fields of application are opening up. Instruments, light, and cameras are introduced into the patient's body through thin guide tubes. The robot holds the devices and performs the necessary movements that the surgeon sets on the console. There are no tremors, no power problems, no lack of visibility of the operating field – because the robot can work in areas that are not accessible with a scalpel in the surgeon's hand. There is always a rule: it is not a device that operates, but an experienced surgeon, but they can be helped to make the operation safer and provide many other possibilities. The so-called telemanipulator does not perform any movements automatically or autonomously. Rather, it is a computer that transmits the movements of the surgeon's hands to microinstruments. Movement is transmitted to the instruments on a five to one ratio. That is, five centimeters of the surgeon's hand movement gives one centimeter of instrument alignment in the patient's body. The instruments move precisely and smoothly.
The robot-assisted intervention method is suitable for almost every patient with prostate disease. The exclusion criterion can only be a history of abdominal surgery if the scars restrict access to the abdominal cavity.
Read more:
Do you need more information about Helios Hospitals or want to schedule your treatment?